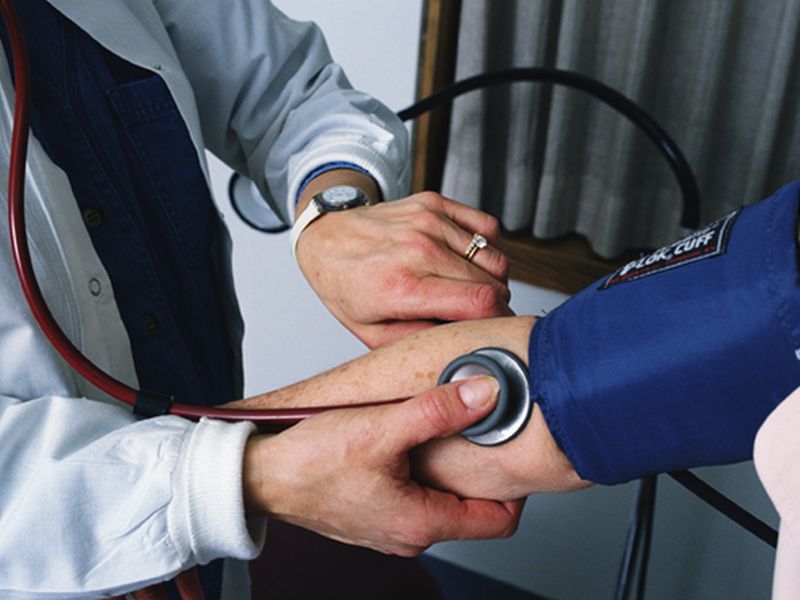
Engaging Americans at high risk for heart disease in aggressive efforts to lower their blood pressure could save more than 100,000 lives a year, a new analysis indicates.
Current guidelines recommend a systolic pressure — the top number in a blood pressure reading — of below 140 mm Hg. But a 2015 study from the U.S. National Institutes of Health suggested more lives could be saved if the goal was less than 120 mm Hg.
The NIH trial known as SPRINT included adults aged 50 and older with systolic readings of 130 to 180 mm Hg and at high risk of heart disease (but not diabetes or stroke).
They had either intensive treatment, with a goal of lowering systolic pressure to less than 120 mm Hg, or standard treatment, with a target of less than 140 mm Hg.
The results were so impressive that the NIH halted the trial early. Risk of death from all causes was 27 percent lower in the intensive treatment group, and death from cardiovascular causes was 43 percent lower for those patients.
What if all U.S. adults with a high risk for heart disease were treated as aggressively? That’s the question that Dr. Holly Kramer, an associate professor of public health sciences and medicine at Loyola Medical Center in Maywood, Ill., and her team sought to answer in the new study.
“I think that people have generally become comfortable with the blood pressure targets that we currently have,” Kramer noted.
Using 1999-2006 health data from a nationally representative survey, researchers determined that 18 million U.S. adults met the criteria of the NIH trial.
Based on an annual death rate of 2.2 percent for that population, they predicted that 107,000 deaths could be prevented each year through intensive systolic blood pressure lowering.
Of the 18 million, close to 9 million had systolic readings at the higher end of the spectrum — 145 mm Hg or greater. And their annual death rate was 2.5 percent. But with intensive control, researchers projected that 61,000 deaths would be avoided each year.
If the results of the NIH trial are correct, “many, many lives would be saved,” said Steven Houser, president of the American Heart Association (AHA). “It’s an interesting prediction.”
Houser is senior associate dean of research at Temple University School of Medicine in Philadelphia.
But how low should the bar be set? Experts are wrestling with that question.
A task force of the AHA and American College of Cardiology (ACC) is expected to issue guidance sometime during the second quarter of 2017.
Dr. Carl Pepine is a past president of the ACC and a professor of medicine at the University of Florida.
Despite SPRINT’s stunning results, Pepine said some European scientists question the findings because the outcomes are based on automated blood pressure readings. In other words, no health care workers were present when blood pressure readings were recorded.
The intent, he said, was to minimize patients’ “white coat,” or stress response, to having their blood pressure taken in a doctor’s office.
“There’s no question that lower is better, but now the actual target level is now open to question,” he said.
There are also potential side effects to lowering blood pressure too far. It can cause dizziness and, potentially, falls and broken bones, particularly in an older population.
But that was not the case in the NIH study, Pepine noted. Patients had frequent visits with clinicians to tweak their medication regimens.
“At the present time, I don’t think there’s a strong compelling reason not to shoot for a lower blood pressure target, even in an older patient, knowing this dramatic benefit that can result,” he added.
The new findings were to be presented Thursday at an AHA meeting on high blood pressure, in Orlando, Fla. Research presented at scientific meetings is considered preliminary until published in a peer-reviewed journal.
More information
For more on controlling your blood pressure, visit the American Heart Association.
Source: HealthDay

Leave a Reply