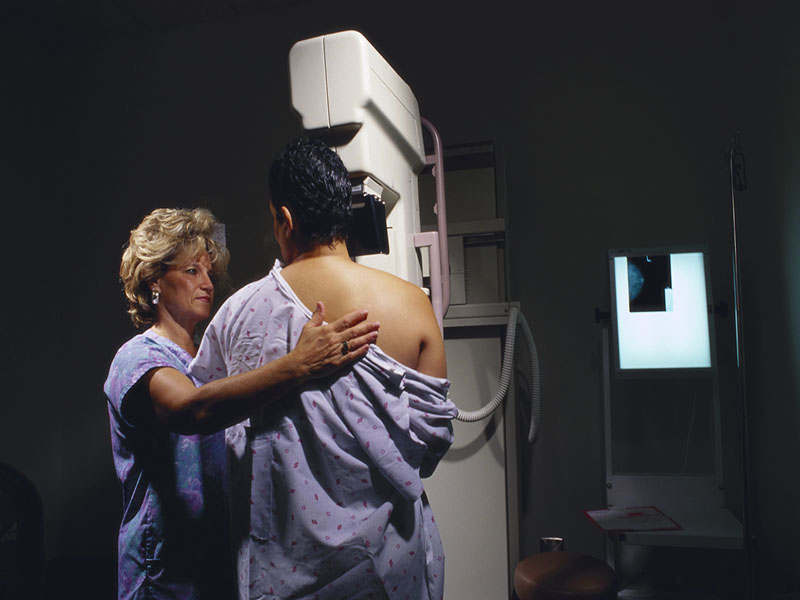
Breast cancer death rates are falling in the United States and many other countries, but increasing in South Korea and some Latin American countries, researchers report.
The investigators looked at data from 47 countries from 1987 to 2013. They found that breast cancer death rates declined in 39 of those nations due to advances in detection and treatment over the past few decades. The largest decrease was in England and Wales, with a 46 percent drop.
In the United States, the breast cancer death rate fell 42 percent. It dropped from 22 deaths per 100,000 women in 1987-1989 to 14 deaths per 100,000 women in 2011-2013, the study showed.
Rates declined in all age groups in the United States: by 50 percent for women under 50; by 44 percent for women between 50 and 69; and by 31 percent for women 70 or older.
There were mixed findings from Latin America. For example, Brazil and Colombia saw rates increase in women of all ages, while in Argentina and Chile, rates decreased in all women.
South Korea had the largest rise in breast cancer deaths, with an 83 percent increase overall. There were higher rates in every age group. However, South Korea’s breast cancer death rate of 5.3 per 100,000 women was still far lower than the U.S. rate of 14 per 100,000 women.
The researchers also found that breast cancer death rates worldwide declined more among women younger than 50 than for those over 50. This is because younger women tend to receive more intense treatment (such as longer courses of chemotherapy) that extends their survival, the study authors explained.
“Breast cancer is by far the primary cancer site in women and, worldwide, represents a quarter of all cancers in women,” said study lead author Cecile Pizot, from the International Prevention Research Institute in Lyon, France.
“Comparing mortality trends between countries helps identify which health care systems have been the most efficient at reducing breast cancer mortality,” Pizot said an American Association for Cancer Research news release.
The impact of breast cancer screening on breast cancer death rates isn’t clear. The study found several cases where nations that were in the same regions and had similar levels of wealth had similar breast cancer death rates even though some had used mammography screening since the 1980s while others introduced it in 2005 or later.
“This finding underlines the difficulty of isolating a single, common factor that would have a major influence on mortality trends,” said Pizot.
“Differences in health care systems and patient management could explain discrepancies in mortality reduction between similar countries,” Pizot said. “However, there is at present little data comparing the management of breast cancer patients across countries.”
The research was to be presented Friday at the San Antonio Breast Cancer Symposium in Texas. Research presented at meetings is considered preliminary until published in a peer-reviewed journal.
More information
The U.S. National Cancer Institute has more on breast cancer.
Source: HealthDay

Leave a Reply