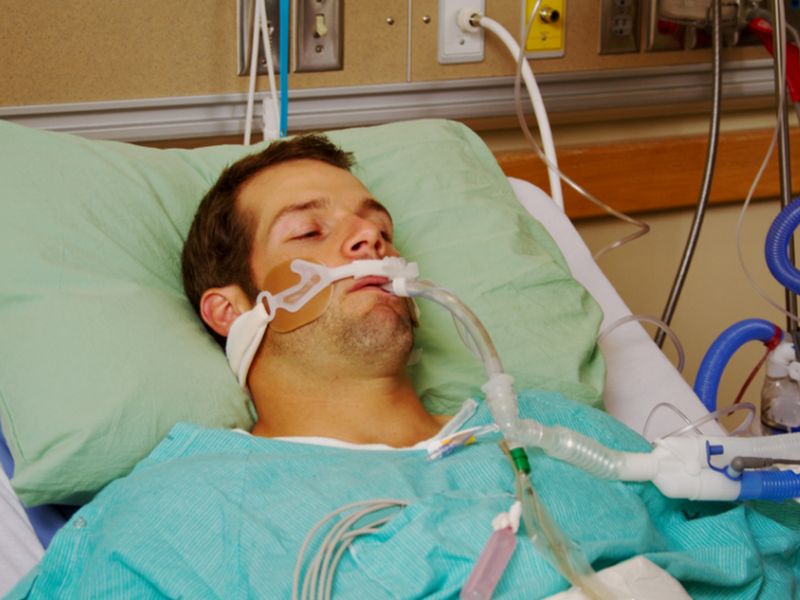
Deadly Legionnaires’ disease is lurking in the water systems of hospitals, nursing homes and long-term care facilities, putting the most vulnerable patients at risk, U.S. health officials said Tuesday.
About 10 percent of people who get Legionnaires’ disease die from it, but in health care facilities the death rate is higher — 25 percent of those patients die if they get the disease, according to a new report from the U.S. Centers for Disease Control and Prevention.
“Legionnaires’ disease in health care facilities is widespread, deadly and preventable,” CDC Acting Director Dr. Anne Schuchat said during a noon press briefing Tuesday.
Despite the CDC’s efforts to get health care facilities to develop effective water management programs, more is needed to protect patients from this deadly bacteria, she said.
Legionnaires’ disease is a serious lung infection that causes pneumonia. People can get it by breathing in small droplets of water containing the Legionella bacteria.
The bacteria thrives in building water systems that are not adequately managed and where disinfectant levels are low, water is stagnant, or water temperatures are warm, Schuchat said.
Most healthy people do not get Legionnaires’ disease after exposure to the bacteria, she said. People most at risk are those aged 50 or older or those who have other risk factors, such as being a current or former smoker, having a chronic disease or having a weakened immune system, Schuchat said.
“People can inhale the bacteria from small water droplets from showers, water therapy spas, baths, cooling towers, decorative fountains and medical equipment, like respiratory therapy equipment,” she said.
Legionnaires’ disease in health care facilities is costly, Schuchat added. In one year alone, insurance companies paid out an estimated $434 million for claims arising from Legionnaires’ disease infection, and total health care costs per patient averaged about $38,000, she said.
The problem is probably bigger than the report’s figures indicate. “It’s just the tip of the iceberg,” Schuchat noted. Most cases of Legionnaires’ disease in health care facilities go unreported because patients who develop pneumonia aren’t routinely tested for Legionnaires’, she explained.
For the report, CDC researchers analyzed 2015 data from 21 areas around the country and found that 76 percent of reported cases of Legionnaires’ disease were linked to health care facilities.
During 2015, approximately 6,000 cases of Legionnaires’ disease were reported to CDC, but only about half included where the infection was acquired.
The findings in this new report are based on data from 20 states and New York City, where how the infection was acquired was recorded.
According to the report, among cases definitely associated with health care facilities:
- 80 percent were tied to long-term care facilities, 18 percent to hospitals and 2 percent to both,
- 72 unique facilities reported cases with the number of cases ranging from one to six in each facility,
- 88 percent of the cases were in people aged 60 or older.
Earlier this month, the U.S. Centers for Medicare and Medicaid Services (CMS) alerted health care facilities that they are now expected to develop and adhere to policies and procedures to reduce the risk of Legionella and other waterborne germs, Schuchat said.
These procedures will be part of future inspections conducted by the CMS, she said.
Dr. Marc Siegel, a professor of medicine at NYU Langone Medical Center in New York City, said, “This is all about improper maintenance, improper sanitation and improper sterilization, and a vastly underreported problem.”
Doctors should be on the lookout for Legionnaires’ disease in patients who develop pneumonia, he said.
Siegel added that the building itself, including its water system, is part of the biosphere of the facility and needs to be as sterile as possible to prevent Legionnaires’ disease.
More information
For more on Legionnaires’ disease, visit the U.S. Centers for Disease Control and Prevention.
Source: HealthDay

Leave a Reply